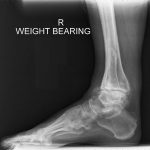
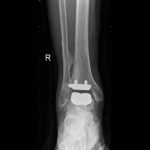
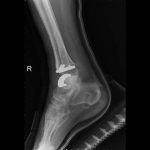
ANKLE ARTHRITIS
What is it?
The ankle joint is formed where the foot and the leg meet. The ankle joint is responsible for the up and down movement of the foot.
The foot moves in two basic directions: in and out and up and down. The ankle joint has nothing to do with the in and out movement of the foot, but approximately 75% but not all the up and down movement is from the ankle.
Arthritis is a broad term for a group of conditions involving damage to the joints of the body. Think of a chicken bone with the end capped with the shiny white glistening cartilage.
Every joint in the body has this cartilage, and when it wears out, arthritis is present.
Initially there is pain followed by stiffness and with time the pain becomes severe. The most common form of arthritis is known as osteoarthritis and is a result of repetitive minor friction to the joint at a microscopic level where the cartilage cells wear out.
Joint problems can also arise from rheumatoid arthritis, gout, ligamentous injuries, trauma to the joint or infection.
The commonest form in the ankle is following an injury or repetitive sprains, also called post traumatic arthritis.
Commonly pain may be the initial presenting symptom. Pain is usually well localized, around the ankle joint but usually it is deep from within the joint. There is a great deal of individual variability in the level of symptoms from ankle arthritis and also the rate at which it progresses. Some people have very little pain with advanced arthritis, and others have terrible pain with lesser degrees of arthritis.
Everyone is different. Generally, symptoms start with pain and perhaps swelling after prolonged standing or high impact type activity. Once the arthritis advances the frequency of pain and swelling also increases.
Treatment is based upon the level of symptoms and degree of arthritis present.
In addition to the physical examination, ankle X-rays and laboratory tests often can confirm the type of extent of the arthritis. Other tests such as a bone scan, computed tomography (CAT) scan, or magnetic resonance imaging (MRI) may be used to evaluate your condition.
Treatment of Arthritis of the Ankle
The requirements of every patient are taken into consideration, and a decision is made which would best suit their lifestyle and needs.
Treatments may include oral medications such as glucosamine, anti-inflammatory medication, steroid injection, synthetic synovium injection into the joint (Synvisc), and orthotic supports such as pads in your shoes or custom-made braces.
Some of these medications work well to alleviate symptoms, and others such as cortisone injection, have a short effect, but work very well to relieve pain for a few months. Unfortunately, the injections cannot be repeated indefinitely, since they eventually stop working.
There are many types of surgery which can be performed. The decision as to which surgery is best for you is based on bone and joint factors such as the quality of the bone, the severity of the arthritis, the presence of any bone or ankle deformity, if the rest of the foot has arthritis or is stiff, and what is the condition of the opposite foot and ankle.
There are also patient factors to take into consideration including your occupation, how much time you spend on your feet, how active your lifestyle is, your exercise interests, your weight, and if you have certain medical conditions such as diabetes which may affect the healing of the surgery.
Surgeries for ankle arthrisis
Arthroscopy may be indicated in the very early stages of treatment only.
The procedure involves two or three small punctures in the front of the joint, and a small telescope is inserted into the joint to remove loose fragments of bone, cartilage or extra bone growth spurs and inflamed tissue.
If the arthritis is minor or at an early stage, a good response to the arthroscopy treatment is noted in about 80% of patients.
Unfortunately, the results of the arthroscopy do not usually last very long, and symptoms return necessitating a bigger operation.
Fusion or arthrodesis is the glueing together of two bones.
The principle aim of this type of surgery is to relieve pain.
Because the ankle joint is responsible for 75% of the up and down movement, with the ankle fused, no further upward movement is present but a limited amount of downward movement still remains after fusion, because of the movement in the joints adjacent to the ankle.
This is important particularly for females, because they are still able to wear a small heel with an ankle fusion despite the limited ankle movement.
The in and out movement of the heel joint is not affected by an ankle fusion.
An ankle fusion is a good operation for certain selected individuals, particularly those with severe bone disease, bone loss or defects in the bone, poor bone quality, and dead bone. Patients who are heavy and who are very active may also be a more suitable candidate for ankle fusion than replacement.
With improved techniques the success rates of ankle fusion have increased, and in particular an arthroscopic minimally invasive procedure of less severe deformities and in patients with high risk of wound sepsis has a success rate is in excess of 95%.
A mini open and a completely open ankle fusion technique should have a success rate of about 97%.
By success I mean that the fusion occurs, and the foot and ankle is in the correct position.
Some rare complications following ankle fusion occur early on due to problems with skin healing and some numbness over the top of the ankle.
The biggest problem with ankle fusion is the development of arthritis in other joints in the foot many years following the ankle fusion.
This is a natural response of the foot joints to the increased stress following the ankle fusion, and can be a serious dilemma, since almost 100% of patients will after a prolonged time demonstrate changes of arthritis in these joints next to the ankle on XR. Not all of these patients have symptoms of arthritis, but for some it can be debilitating, since the only option remaining is to fuse these joints as well resulting in considerable incapacity.
When an ankle joint is fused, there is of course no up and down movement in the ankle. There does however remain for some patients a limited amount of up and down movement which occurs in the adjacent joints.
Exercise is possible following an ankle fusion, and includes walking, hiking, golf, biking, and for some patients skiing and double tennis. There are restrictions noted by all patients because of the stiffness, particularly with activities which require bending movements, including yoga, pilates, crouching and all ball or racquet sports.
The goal of ankle replacement is to maintain or improve the natural movement of the ankle. From a standpoint of day to day activities, there is far better function with an ankle replacement than that of a fusion (where the joints are glued together).
The history of ankle replacement when it was first performed in the early 1980’s was not good at all and was associated with a high rate of failure. This failure was largely due to the incorrect designs of the prosthesis, and the design of the implants has improved considerably over the last 30 years, making ankle replacement a far more realistic operation for surgeons to offer their patients for treatment of ankle arthritis.
The results of ankle replacement today are good, but what do we mean by this statement?
The aim of the surgery is to improve or retain the movement in the ankle, and therefore improve the function compared with fusion.
However, ankle replacement surgery is complex.
A significant learning curve exists and even experienced surgeons have found that it takes time for them to learn how to perform this surgery. It may take many years for a surgeon to gain sufficient experience to perform the surgery and to be able to predictably limit the potential for complications.
Recent scientific reports have outlined this problem in more detail, and even though I was taught in the United States by Dr. Meyerson who has extensive experience with this surgery and has performed over 1000 ankle replacements using various implant designs, complications of surgery still occur.
The main advantage of total ankle replacement is the return of some freedom of movement in the ankle.
This movement is important for walking smoothly, exercise and all bending type of activities. Full movement of the ankle joint is never regained even with total ankle replacement.
The movement that is present, however, is far preferable to the lack of movement in the fused ankle. There is another very important aspect to ankle replacement in that it avoids the stresses that occur following ankle fusion.
I currently use one type of ankle implant or prostheses.
The SALTO-TALARIS ANKLE SYSTEM with great success.
This implant was originally designed and used in Europe, and has been implanted with very encouraging results. The Salto ankle replacement differs in a number of respects from the Agility ankle, in that it does not include gluing together the fibula to the tibia, and has a better coverage of the implant on the talus surface and is considered a more anatomic procedure than other implants.
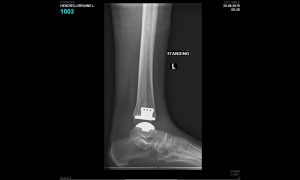
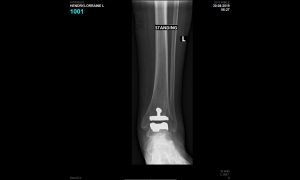
This is a graphic illustration of the Salto ankle prosthesis on the left and XR of the prosthesis in the ankle following the surgery for a patient with traumatic arthritis.
Another type of ankle replacement which can be used is a custom designed prosthesis, which is tailored for each patient by means of 3D printing based on CAT scan and MRI images on specific occasions.
It is used when the bone quality is poor, when there is dead bone (called avascular necrosis or AVN), and when the patient has an increased risk of the prosthesis sinking or subsiding into the bone.
Unlike other regular implants, this custom prosthesis has a long stem which fits into the heel bone (the calcaneus). This has been an extremely useful prosthesis for patients who have previously undergone an ankle replacement which has failed due to sinking in of the implant due to poor bone disability.
The decision to perform an ankle replacement is based on a joint discussion between you the patient and myself.
The real issue for a patient making a decision between an ankle fusion and an ankle replacement is the increased potential for complications following ankle replacement.
There are unfortunately also increased complications of the healing process with ankle replacement compared with fusion, including a higher incidence of the wound healing and skin problems, loss of feeling on the top of the foot, fracture of the ankle bones, and infection.
The results that Dr Meyerson has, indicate that there is an 80% success rate at 10 years following ankle replacement. This means that the patient has an 80% likelihood of having the same ankle prosthetis in at 10 years with good function. This also means that there is a 20% possibility that a revision of surgery may have to be performed, and this may include another ankle replacement, or an ankle fusion.
The recovery following the total ankle replacement is very carefully monitored.
Rehabilitation and exercise are essential. My approach to rehabilitation includes an exercise bicycle and therapy in a swimming pool beginning as soon as the cast is removed and the incision is healed.
This is followed by a very strict course of physical therapy exercises which improve the range of movement and ultimately improve the final outcome of the joint replacement procedure.